
Day 22
We've decided to start a blog with updates and pictures of Teagan throughout this journey as a journal for our thoughts and a better way to share them with our friends and family. Beginning this on day 22 of our hospital stay and day 23 of Teagan's life will require some catching up but I'll do my best!
 Teagan was born on Friday March 21st 2008, "Good Friday!" at 12:51pm at Kadlec Medical center in Richland, WA. She was 19 inches long, 6 lbs. 13 oz and scored a 9/9 on her apgars! I was 39 weeks pregnant and scheduled for a repeat c-section due to a prior c-section with our first son Gavin. Looking back we are so thankful that she did not have to endure a stressful labor/delivery and was able to come into this world as strong as possible! Unaware of her condition, I was able to 'room in' with her after delivery and had the chance to hold her and nurse her several times. Around 1am Saturday morning, I asked the nurse if she would give Teagan a bottle for her
Teagan was born on Friday March 21st 2008, "Good Friday!" at 12:51pm at Kadlec Medical center in Richland, WA. She was 19 inches long, 6 lbs. 13 oz and scored a 9/9 on her apgars! I was 39 weeks pregnant and scheduled for a repeat c-section due to a prior c-section with our first son Gavin. Looking back we are so thankful that she did not have to endure a stressful labor/delivery and was able to come into this world as strong as possible! Unaware of her condition, I was able to 'room in' with her after delivery and had the chance to hold her and nurse her several times. Around 1am Saturday morning, I asked the nurse if she would give Teagan a bottle for her  next feeding as I was very sore and needing a few hours of rest. A few hours later the nurse returned without Teagan and explained that she
next feeding as I was very sore and needing a few hours of rest. A few hours later the nurse returned without Teagan and explained that she noticed a rapid breathing rate and heart rate after taking her to feed her. The NICU staff examined her and did some chest x-rays and thats when they noticed her enlarged heart. After performing an echocardiogram they noticed some problems with her left ventricle and left aortic valve. The results of the tests were sent to spokane to be evaluated by a pediatric cardiologist and Teagan was intubated and an IV was started to give her a medicine called
 prostaglandin (which helps her heart function much like it had been in utero.) Early saturday morning we got the preliminary diagnosis on her condition called "Critical Aortic Stenosis." In Teagan's case, her left ventricle failed to form completely and is thickened which inhibits it from properly pumping. Also, her aortic valve is very small and is not properly functioning either. We were told that she would need some sort of surgery to correct her defect, and until then she would need the Prostaglandin to keep her alive. We were given the option of transferring her to Sacred Heart hospital in Spokane, or Children's hospital in Seattle. After choosing Children's in Seattle they told us that she would be flown there sometime that afternoon and that Trent was allowed to fly with her but I would have to stay in the hospital until atleast Sunday. (48 hrs. post surgery) The airlift team arrived shortly after 12 noon and they were on their way by 2 pm. I was released from the hospital in Richland Sunday around noon and after filling a few prescriptions and packing, was on my way to Seattle.
prostaglandin (which helps her heart function much like it had been in utero.) Early saturday morning we got the preliminary diagnosis on her condition called "Critical Aortic Stenosis." In Teagan's case, her left ventricle failed to form completely and is thickened which inhibits it from properly pumping. Also, her aortic valve is very small and is not properly functioning either. We were told that she would need some sort of surgery to correct her defect, and until then she would need the Prostaglandin to keep her alive. We were given the option of transferring her to Sacred Heart hospital in Spokane, or Children's hospital in Seattle. After choosing Children's in Seattle they told us that she would be flown there sometime that afternoon and that Trent was allowed to fly with her but I would have to stay in the hospital until atleast Sunday. (48 hrs. post surgery) The airlift team arrived shortly after 12 noon and they were on their way by 2 pm. I was released from the hospital in Richland Sunday around noon and after filling a few prescriptions and packing, was on my way to Seattle.  Seeing Teagan in the ICU for the first time when I arrived in Seattle was heartbreaking. She was resting comfortably in her little bed with a thousand wires and tubes going everywhere. Its all pretty overwhelming at first, but the nurses were great and explained what every wire was for and that she was comfortable and not in any pain. Understanding what was happening and why she was hooked up to certain things made it much easier to bear. Over the next few days we met with the cardiac team to discuss the best options for Teagan. At first it was thought that she was a good cadidate for a femoral artery balloon catheter procedure in hopes that the aortic valve could be 'popped' open and therefore able to function somewhat normal. But after some tests and ultrasounds it was determined that her arteries were too small to support the procedure and that her left ventricle was incapable of properly pumping even if the valve was to open up. The only other option left was open heart surgery, which was a terrifying thought. Trent and I had little knowledge about the anatomy of the heart and how amazing and complex it is. But after meeting with the docs and going over numerous heart diagrams, each of us could probably pass a pop quiz in anatomy/heart structure! The procedure decided upon is called the Damus-Kaye-Stanzel in which they fuse the aortic & pulmonary valve and widen one of her ducts to
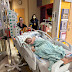
Seeing Teagan in the ICU for the first time when I arrived in Seattle was heartbreaking. She was resting comfortably in her little bed with a thousand wires and tubes going everywhere. Its all pretty overwhelming at first, but the nurses were great and explained what every wire was for and that she was comfortable and not in any pain. Understanding what was happening and why she was hooked up to certain things made it much easier to bear. Over the next few days we met with the cardiac team to discuss the best options for Teagan. At first it was thought that she was a good cadidate for a femoral artery balloon catheter procedure in hopes that the aortic valve could be 'popped' open and therefore able to function somewhat normal. But after some tests and ultrasounds it was determined that her arteries were too small to support the procedure and that her left ventricle was incapable of properly pumping even if the valve was to open up. The only other option left was open heart surgery, which was a terrifying thought. Trent and I had little knowledge about the anatomy of the heart and how amazing and complex it is. But after meeting with the docs and going over numerous heart diagrams, each of us could probably pass a pop quiz in anatomy/heart structure! The procedure decided upon is called the Damus-Kaye-Stanzel in which they fuse the aortic & pulmonary valve and widen one of her ducts to  allow for increased blood flow as well as a few other adjustments. It's basically bypassing the left side of her heart, since her left ventricle cannot function. She has a single ventricle that works- her right. This is a temporary "fix" for Teagan though. She will out grow this procedure, then in 4-6 months, she'll have another surgery called the Bi-Directional Glenn. Her last surgery, which will finish the replumbing of her heart will be between 4-6 years of age and it's called the Fontan. This series of 3 surgeries is referred to as the "Norwood" track. We got the word on Tuesday March 25th that surgery was scheduled for Thursday morning at 7am, Teagan would be 6 days old. It was a relief knowing that there was a plan in place to repair her heart but also very scary having an actual date and time. Somehow it became much more real that all of this was really happening.
allow for increased blood flow as well as a few other adjustments. It's basically bypassing the left side of her heart, since her left ventricle cannot function. She has a single ventricle that works- her right. This is a temporary "fix" for Teagan though. She will out grow this procedure, then in 4-6 months, she'll have another surgery called the Bi-Directional Glenn. Her last surgery, which will finish the replumbing of her heart will be between 4-6 years of age and it's called the Fontan. This series of 3 surgeries is referred to as the "Norwood" track. We got the word on Tuesday March 25th that surgery was scheduled for Thursday morning at 7am, Teagan would be 6 days old. It was a relief knowing that there was a plan in place to repair her heart but also very scary having an actual date and time. Somehow it became much more real that all of this was really happening. 
Thursday morning came and Trent and I arrived at the hospital early to spend some time with her prior to her going back. The nurses said that she was doing fairly well, but she was definitely ready to have surgery as she was having a hard time maintaining her SAT levels (blood oxygen) and her breathing was rapid indicating her heart was having to work extra hard. We were able to walk with her down the hallway to the entrance of the surgical wing and then had to say goodbye. This was probably the single hardest moment for me over the whole 3 weeks that we've been here now. Trent and I were given a pager and told that we would receive 4 pages throughout the surgery to let us know where they were at with the procedure. The 1st page indicated that anesthesia was finished and they were beginning surgery. The 2nd page was when they started her on the heart/lung bypass machine. The 3rd page meant she was off the bypass machine and thus the surgeons were finished. The 4th page meant that she was on here way to recovery. The surgery was expected to last until mid-afternoon, but we got the news around noon that she was on her way to recovery! Everything went well and there were no complications with the procedure. We were able to see her around 3:30 once she had been moved back to a room in the Cardiac ICU area. The dr.'s had to leave her chest open after surgery to acccomodate any swelling in the days following surgery and placed a thin film over the opening where we could see the outline of her tiny heart beating. She was pretty sedated and intubated but overall doing well for the surgery that she had just been through.
In the days following surgery, she had one episode of v-tach (irregular rapid heart rythm) and had to be put on a pacer for one night. She also required a large amount of fluid post op, to lower her heart rate which had soared to the 190's. (normal range for her size is 120-150's). She was so swollen in the few days post op that she didn't even look like our baby. But we were reassured that as soon as she started flushing the fluid out on her own they could start a diuretic medication to help her and she should return to normal size.
Her chest was closed on the monday following the surgery (april 1st, day 10) This surgery also went well and we were excited to have her last 'procedure' behind us hopefully. She has since been extubated (breathing tube removed) and had her chest drain tube removed as well as her pacer wires.
In the last week her breathing and heart rate have increased and she had to be put on a C-pap machine (positive air pressure) to help her breathe. There was talk of a possible infection and we are still watching her blood culture results daily. She has also developed a painful sore on her left wrist from an iv that was in place. The dr.'s are not sure why it is so swollen and red and have done x-rays to determine if part of the iv catheter has broken off in her wrist and is causing an absess. We are watching it very closely and there has been no decision made yet on what the plan is. She is however being weined off of her c-pap machine and as of today (april 12th ) she's been breathing on her own for 19 hours! We are still in the ICU area of the hospital until her heart rate and breathing are more under control. She's receiving my milk via a feeding tube through her nose, and is taking full feeds already! I am very anxious to begin oral feeds as soon as possible, and on monday someone is coming by to help with that!
We will try to post on here as often as possible. Sorry this first one was so long! Thank you all for your continued support and prayers throughout this whole journey, keep them coming! God has his hands on her and reveals himself more to us each day through our sweet baby girl. We are so thankful to have been given this gift in her and can't wait to bring her home!!


















5 comments:
Trent & Susie,
My heart goes out to you both...I can empathize with your every word. Teagan is such a little doll and before you know it, you'll have her home. Remember that we're refined through fire and that God is there, each step of the way. He's chosen you to endure this and a true gift He's given you...Teagan. We're keeping you in our thoughts and prayers and look so forward to future "playdates" with our little girls! We're so thankful that
Maddie will have someone like her to relate to...they can share their "zippers" someday!
Our Love,
Bryan, Katie & Maddie Allred
Royal City, WA
PS- Love your blog & so glad you created it! I'll keep checking for updates!!! Take Care!
We love you and are thinking of you and Baby Teagan is in our everyday prayers. Stay stong, she is truly a gift and blessed to have such a strong family. Your home town is praying for you. Love Always, Chris, Danny, Alyssa and Dylan Liliensiek
Trent and Susie,
Thank you for creating this blog, you have allowed so many of us to be a part of your life and Teagans, what a Blessing you have given us!
We love you and can't wait for Emma and Teagan to grow up and play "dress up " together.
God continues to bless you all!
You have our prayers and the prayers of so many.
love, Erica, Paul, Lily, Nicholas and Emma White
Twisp, Wa
Trent, Susie...just looked at the latest pics of Teag with you two. She is SO CUTE...gonna be just like Gavin. You guys sure come up with the good lookin' ones. Hoping big time that heart rate settles down and oral feeding prep begins and YOU both get sleep. Love ya, Janie
Hi Susie (& TRENT)
I haven't talked to you in a very long time but Chris has given me some updates. I just wanted to say hi and wish your family the best. Your family will be in my prayers. Both your children are beautiful!!! God Bless!
Katie Eckles
Post a Comment